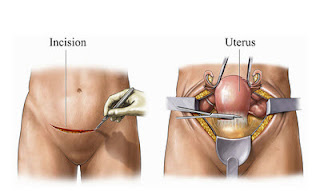
Once I made the decision, it was easy to schedule the surgery. I chose the traditional method rather than the laparoscopic, because the procedure was a shorter duration, and I had already decided whom I wanted as my surgeon.
 The hospital and staff treated me well from the moment I was admitted. The prep part went smoothly, and I was under sedation quickly and easily. Then I woke up. I chatted and joked with the nurse, who was administering morphine to keep my pain levels manageable. Pain was okay with the meds, as long as I didn't laugh or breathe too deeply. I had no sense of time, so I'm not sure how long I stayed in the recovery room. At some point, I was transferred to the room in which I'd stay the next two nights. I didn't like the moving part, especially when the gurney went over thresholds. I'm not going to sugar coat it, it hurt like hell, with a side of barbed wire. The gentleman who was stuck with transporting me felt awful for torturing me, and gave me time after crossing each of the nine threshold to breath through the pain.
The hospital and staff treated me well from the moment I was admitted. The prep part went smoothly, and I was under sedation quickly and easily. Then I woke up. I chatted and joked with the nurse, who was administering morphine to keep my pain levels manageable. Pain was okay with the meds, as long as I didn't laugh or breathe too deeply. I had no sense of time, so I'm not sure how long I stayed in the recovery room. At some point, I was transferred to the room in which I'd stay the next two nights. I didn't like the moving part, especially when the gurney went over thresholds. I'm not going to sugar coat it, it hurt like hell, with a side of barbed wire. The gentleman who was stuck with transporting me felt awful for torturing me, and gave me time after crossing each of the nine threshold to breath through the pain.My nurses were outstanding. I was up and walking in no time, and they were with me every step of the way. I was given lots of advice before surgery, and I want to share the hints and tricks that worked best for me. The best advice was to suck it up, and stretch out. Don't give in to clutching a pillow to your tummy. When it's time to walk, stand up straight and breathe through the pain. I took the "suck it up" advice, and I know the intensity and duration of pain was greatly reduced because of it. Essentially, it's like ripping off a band aid. You can go slowly, and prolong the pain, or you can rip it off and get it over with. I chose the latter.
Things I enjoyed doing before surgery were unpleasant for a while after surgery. Laughing, taking deep, cleansing breaths, going from laying down to sitting to standing, and vice versa. Each day, the pain lessened and it wasn't long before I was driving. I am not ashamed to sat how painful navigating speed bumps were. Yes, I drove slowly and cautiously in general, and I crawled over speed bumps in particular. I loved being mobile, but I was careful to follow another piece of advice: don't do too much too quickly. I was (mostly) pretty careful about not overdoing it.
I was struck with a stark reality about 1/2 through my recovery: there's an empty spot in my body cavity. I felt all sorts of things, depression, fear, and incomplete, for a while. I was expecting it, so I knew what these feeling were when they crashed over me. I was worried for a while that I wouldn't be able to enjoy an active sex life as I had before. I was afraid that I had mutilated my body and would no long experience orgasm as I once did. I can assure you, that fear is groundless. My missing parts and pieces do not in any way reduce my sexual appetite or the ability to experience pleasure.
There are a lot of articles and information out on the interwebs, but I'm not going to link to any of them, as I didn't find the concerns they raised either true or helpful. My hysterectomy experience went well, and I achieved the desired results: I no longer have uterine pain from fibroids.
I take a daily estrogen supplement, and I am free of menopausal symptoms. All in all, I consider my hysterectomy a success.


